Latest news
Find out more about our work by reading our latest news stories and insight articles.
Media enquiries
Publications
Featured article
30 November 2023
How do advance market commitments and volume guarantees shape healthcare markets?
In an ideal world, markets function perfectly. Buyers and sellers trade goods and services. Production and consumption are efficient. In reality, market failures and inefficiencies exist. The impact of these market failures is stark in healthcare, compromising public health outcomes and increasing patient morbidity and mortality. Market-shaping interventions can enable…
Read moreFilter stories

25 April 2024 | News
UK improves access to life-saving malaria drugs
Support for MedAccess will be used to negotiate lower prices for vital malaria drugs and diagnostic tests for people in…

26 March 2024 | News
MedAccess welcomes rollout of G6PD testing and tafenoquine in Brazil
MedAccess today welcomed news from Brazil that people from the Yanomami Indigenous Territory in Roraima will become the first to…

20 March 2024 | Insight
Do you speak market shaping? Reflections from the first Global Health Market shaping conference
Market shapers gathered in Barcelona earlier this month for the first ever Global Health Market Shaping conference. MedAccess colleagues and…

4 March 2024 | News
Alison Evans and Anil Soni join MedAccess Board
MedAccess today announced the appointment Alison Evans and Anil Soni to the Board of Directors. Alison and Anil bring deep…

7 February 2024 | News
Keeping impact at the heart of MedAccess’ investment decisions
MedAccess has underlined its commitment to putting impact at the heart of its investments by signing up to the Operating…
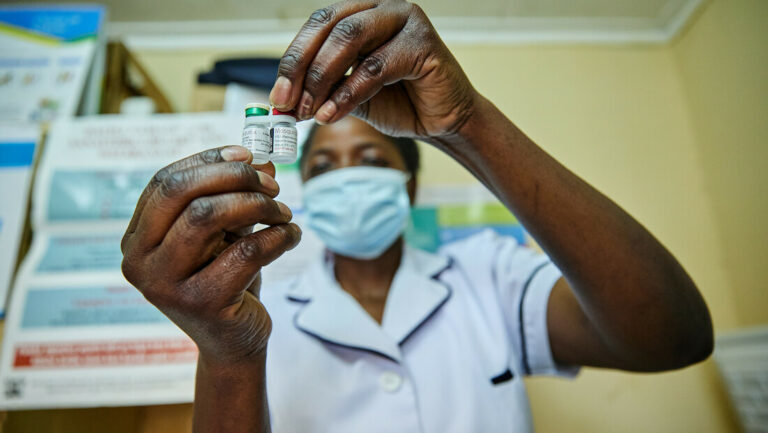
22 January 2024 | News
Malaria vaccine introduction “a big step forward for global health”
MedAccess today warmly welcomed news that Cameroon has started protecting its children against malaria as part of the country’s routine…

30 November 2023 | Insight
How do advance market commitments and volume guarantees shape healthcare markets?
In an ideal world, markets function perfectly. Buyers and sellers trade goods and services. Production and consumption are efficient. In…

13 October 2023 | News
MedAccess congratulates Uganda’s efforts to increase access to HIV self-testing
Uganda has become the first country to adopt HIV self-tests procured under the terms of MedAccess’ volume guarantee to Guangzhou…

11 October 2023 | News
Antony Ross OBE appointed Chair of MedAccess Investment Committee
MedAccess today announced the appointment of Antony Ross to its Board of Directors and as Chair of its Investment Committee.…



















