Access to healthcare: a daily emergency
Every day, millions of people are unable to access medical innovations that could protect their lives and improve their health. Despite decades of progress, many healthcare products remain unavailable or unaffordable for people in low- and middle-income countries.
We live in a golden age of medical science. But more than two billion people can’t access medicines, vaccines and new technologies, causing preventable illness, disease and death.
The world has become numb to a daily emergency
Every day, millions of people face illness and death because they cannot access the medical innovations that would protect, diagnose, treat or cure them.
This is a daily health emergency. But it is one that has been going on for decades. The problem is so large and persistent that the world has become numb to it.
Huge inequalities exist in access to healthcare. People living in high-income countries usually have access to the medicines they need when they need them. Those same medicines might not reach people in low- and middle-income countries for years or even decades. And if they are available, they may be in limited supply or at a price that is unaffordable.
Until we bridge the gap between makers and buyers, lifechanging health products will remain out of reach for billions of people.
What it means for healthcare providers
Being able to prescribe the right medicine at the right time is essential for healthcare providers.
If products are in short supply, doctors often spend time looking for alternatives or, in some cases, tailoring completely different treatment plans. This takes time and reduces the number of patients a doctor can see in a day.
Lack of availability also undermines doctor-patient relationships. These relationships are vital for compliance with treatment plans as the patient must have confidence in the doctor and that the plan will work.
When doctors are unable to prescribe the medicines a patient needs, they are more likely to become discouraged and potentially seek other, less effective, options.


Why products aren’t available
Every day, new medical innovations are being developed. But too often they do not reach the people who would most benefit from them. For people to be able to access health products, they must be available in their country, there must be enough supply, and they must be able to afford them.
Manufacturers often decide not to make products available in markets they consider risky because of inefficiencies or instability. If a product is not registered in a country then it cannot be prescribed or sold there legally.If a manufacturer enters a market it considers risky, it will often allocate smaller volumes, especially when there is no robust visibility on current and future demand.
Finally, even when products are available, they may be priced too high, making them unaffordable for patients, procurers, or governments. The human cost of inefficient markets is people missing out on healthcare products that can protect, save, and improve their lives.
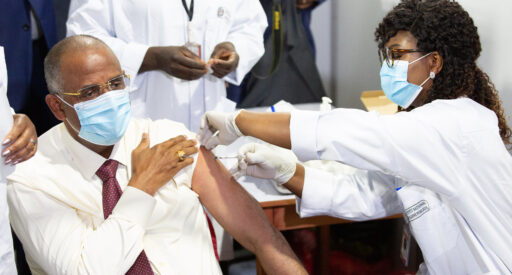
Lessons from COVID-19 vaccination
The COVID-19 pandemic drew global attention to the glaring inequalities in access to healthcare. From the first weeks of the outbreak, high-income countries hoarded clinical supplies, reducing availability and driving up prices for essential equipment.
COVID-19 vaccines were developed and produced at unprecedented speed. But distribution was unequal. People in high income countries received booster shots before tens of millions of people in countries in Africa had even received a first dose.
As the supply situation improved, we began to see what was possible.
COVAX, a global partnership focused on development and distribution of COVID-19 vaccines, made more doses available to 92 of the lowest income countries in the world free of charge through the COVAX Advance Market Commitment. This led to a smaller coverage gap between low- and high-income countries than for any other vaccine.
COVID-19 has also increased the focus on regional vaccine manufacturing. A geographically diverse vaccine manufacturing base would reduce the risk of low- and middle-income countries being at the back of the queue for new vaccines, whether in a pandemic or for routine immunisation.